Nutrition Administration Through Nasogastric Tube
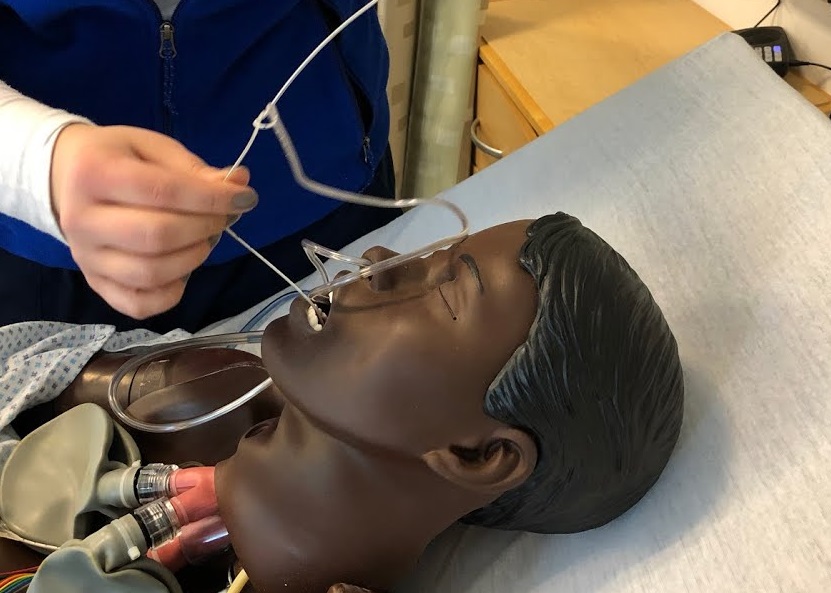
Common Nursing Problems and Interventions
Maria Helena Palucci Marziale,
* Lilian Sheila de Melo,
** Maria Helena Larcher Caliri,
*** Denise de Andrade
* Free Teaching Professor at the Ribeirão Nursing School
Preto/University of São Paulo – Brazil
** Nurse.FAPESP Scientific Initiation Scholarship – Brazil
*** Doctor Professor at the School of Nursing of Ribeirão Preto/University of São Paulo – brazil
marziale@eerp.usp .br
Summary
Feeding through a gastric tube is a procedure frequently performed by nurses who must be trained not only for execution of the technique of insertion of the tube and administration of the diet, but also to intervene in the event of complications.This is a descriptive study whose objective was to identify, find out, among hospitalized patients who received feeding through the nasogastric tube, the complications presented and identify the interventions carried out against these complications.The data were collected through an interview with 85 patients and through consultation of their medical records.The most frequent complications found were gastrointestinal followed by mechanical complications (tube leakage and obstruction).Most of the nursing interventions were related to decreasing the infusion rate and suspending the diet, inserting another tube, hygiene care, and patient comfort.
Keywords :nursing care, nasogastric tube, tube feeding.
Abstract
Nasogastric tube feeding is a procedure frequently done by nurses to which they need to be prepared not only to do technical procedure of inserting the tube and patient feeding but also to intervene should complications occur.Descriptive study had as its goal to identify patients with nasogastric tube feedings, complications presented and nursing intervention done related to complication.Data was collected through interviews with 85 patients and through patient’s records.The most common complication were gastrointestinal followed by mechanical (tube obstruction and displacement).Common nursing interventions were directed to slow the rate of diet infusion, interruption of diet, placement of new tube and nursing care related to hygiene and comfort of patient
Key words:nursing care, nasogastric tube, tube feeding.
Summary
Nasogastric tube feeding is a frequently performed procedure As a nurse, he or she must be trained not only to perform the probe installation technique and diet administration, but also to intervene in the event of complications.Descriptive study whose objective was to find out, among hospitalized patients who received food through a nasogastric tube, what complications occurred and to identify the interventions carried out before the complications.The data were collected through interviews with 85 patients and through documentary consultation of medical records.The most frequent complications found in the gastrointestinal tract are followed by mechanical complications (tube leakage and obstruction).The most frequently performed sick interventions are related to reducing the rate of infusion and suspending the diet, installing another probe and hygiene care.
Keywords: sick care, nasogastric tube, tube feeding.
Introduction
Enteral nutrition is a nutritional alternative with both physiological and economic benefits in which nutrients are administered directly into the tract gastrointestinal tract providing adequate nutritional support to patients who have normal digestion and absorption processes, but who for some reason do not complete their nutritional needs orally.(1)
Within The reasons why the patient needs enteral nutrition include: vascular cerebral event, coma, multiple sclerosis, trauma, patients undergoing chemotherapy or radiotherapy, hypermetabolic patients, transition from parenteral to oral nutrition, patients on mechanical ventilation, gastric and esophageal cancer. , maxillofacial surgery, inflammatory disease of the esophagus and intestine, biliary tract disease, short bowel syndrome, presurgical preparation, burns, anorexia, cardiac cachexia, decreased gastric evacuation and gastrointestinal surgery.(2)
Enteral nutrition has been associated with gastrointestinal, mechanical, pulmonary, metabolic, and psychological complications.(1,3) Gastrointestinal complications include diarrhea – which may be caused by drug therapy, poor nutrition, and hypoglycemia. -albuminemia, type of formula, bacterial contamination of the formula, rapid infusion of the diet, lactose intolerance, altered gastrointestinal flora.Inadequate gastric emptying and abdominal distension – caused by gastrointestinal tract dysfunction, type of formula (high lipid content), rapid infusion, lactose intolerance, large volumes of diet.Gastroesophageal reflux – caused especially by large caliber tubes, greater than 12 Fr.(3-5)
Mechanical complications, which are associated with tube problems include tube obstruction;accidental exit or migration of the probe – caused by altered peristalsis, hyperactive patient;nasal erosion, necrosis and abscess of the nasal septum.Acute sinusitis, hoarseness, otitis, esophagitis, esophageal ulceration, esophageal stenosis, tracheoesophageal fistula and esophageal perforation.(6)
Pulmonary complications include pulmonary aspiration, hydrothorax, pneumothorax, pulmonary hemorrhage, empyema, bronchopleural fistula, pneumonia and subcutaneous emphysema.(7)
Among the metabolic complications, we find dehydration, diarrhea, hyperglycemia, hydroelectrolyte imbalance, infection and kidney dysfunction.Psychological complications are derived from the lack of stimulation to the palate, the unattractive and routine presentation of food and low self-esteem, which can cause anxiety and depression.(1)
Several complications are associated with the caliber of the nasogastric tube (NGT), for example, large caliber tubes can cause pharyngitis, otitis, tracheoesophageal erosion, incompetence of the esophageal sphincter, stenosing ulceration of the larynx, excoriations of the nose and sinusitis , among others.Seeking to reduce or prevent these complications, small-caliber flexible and soft probes were made available, which are difficult to insert and easy to migrate.(8)
Complications derived from The use of NGT can be avoided if there is a well-prepared nursing team to care for the patient, since they are responsible for everything from choosing which probe to be inserted to providing care for the reactions presented. by the patient.Thus, the nurse must proceed according to data from the literature as follows:(1,3,5,6,8)
• Verify the position of the probe through abdominal auscultation (inject 5 to 20 ml of air into the probe while listening to the epigastric area with a stethoscope) and aspirate the gastric contents (this can be confused with pleural fluid – check the pH, if it is acidic it is gastric fluid, if it is basic it is pleural or intestinal fluid).
• Evaluate the patient’s neurological status: confusion, disorientation, agitation, since these states can cause displacement of the probe.
• Check the tolerance of the diet by measuring the gastric content, if it is greater than 150 ml, reintroduce the liquid into the stomach and suspend the diet.High residue indicates difficulty in gastric emptying and may cause bronchoaspiration.
• Wash the tube with water after administration of diet and medications in order to avoid obstruction of the tube.
• Keeping the patient in an elevated position, 30o – 45o decreases the risk of aspiration in case regurgitation and vomiting occur.
• Monitor weight, signs of edema and dehydration, frequency of evacuations and glycemia.
The traditional criteria for verifying the position of the tube are not reliable in patients in critical condition for the following reasons: abdominal auscultation of insufflation Air can be confused with air bubbles in the pleura, lung and esophagus and what is aspirated can be of pleural origin or bronchial secretions.For these reasons, it is recommended to verify the position of the tube by means of abdominal or chest responsibility of the nurse in this process, we were interested in investigating what are the most commonly observed complications in patients with enteral therapy and what is the action of nurses in each situation.
Objectives
Find out among patients who receive feeding through a nasogastric tube what complications occur.
Identify the nursing interventions, documented in the medical history, in the face of such complications.
Methodology
Descriptive research carried out in two execution phases: the period between March 2000 and February 2001.The identified studies were analyzed with a view to identifying possible complications and the nursing interventions carried out.
In the second phase, observation was carried out on 85 patients who were receiving feeding through a nasogastric tube and subsequent documentary analysis of the medical records seeking to identify possible complications and nursing interventions carried out and recorded in the history.
Place: patients who were receiving nutrition through the NGT at the University Hospital of the Ribeirão Preto- São Paulo- Brazil.
Sample and selection criteria: 85 adult patients of both sexes who were receiving nutrition through the NGT, in the period from March to December 2000 and who agreed to participate in the research.
To collect data, an instrument was used that contained closed questions related to the identification of the subject and data regarding the indication of the tube diet, type of tube, substances administered through the tube, signs and symptoms recorded in the medical history that indicated complications.The instrument was evaluated and accepted by three nursing researchers in relation to the objectivity of the content.
The research project was approved by the research ethics committee of the hospital hosting the study.The subjects in the sample issued informed consent when they were unable to do so, which was signed by the person responsible for the patient.
Results and Discussion
Table 1 shows the data of identification of the subjects.We can see that 58% of the patients belonged to the male sex and 41.2% to the female sex;The age group with the highest occurrence of use of the nasogastric tube for feeding was between 65 and 75 years, a fact that may be associated with the pathologies of the elderly.The predominant profession was retired/inactive (34.1%) followed by housekeeping (25.9%).


In relation to the medical diagnoses attributed for the indication of NGT feeding, table 2 shows the results.


We can observe In this table, the situation of inability to digest food is the one with the highest number of diagnoses indicative of the use of NGT (54.1%).Diagnoses related to the inability to meet nutritional needs were responsible for 20 indications (23.6%) of the use of the nasogastric tube for feeding and diagnoses related to the inability to absorb food were responsible for 18.8%. of cases.
The main diagnoses, described in the literature, that require enteral tube feeding,(1,3-5) are related to the following situations: cerebral vascular accident, multiple sclerosis , head trauma, hypermetabolism, malnutrition, esophageal or stomach cancer, oral or dental surgery, coma, pancreatitis, inflammatory bowel disease, short bowel syndrome, burns, depression, anorexia nervosa, face and jaw injury, oral cancer, decline of gastric emptying, digestive fistula and multiple trauma.
The period of use of the nasogastric tube varied from 1 to 107 days, as shown in table 3. In this table the period of use of the SNG was variable and some patients used it for more than 60 days.This tube is the most comfortable and best tolerated by the patient because it is soft and flexible; however, position evaluation is more difficult and migration is easier.(3)


According to the studies on the incidence of tube obstruction due to the diameter of the probe, no significant differences were found in relation to the type of tube material, it was found that those of Polyurethane are responsible for the greater number of occlusion than silicone.The nasogastric tube is used for the administration of food (41.2%), food and drugs (57.6%) and drugs only (1.2%).
When association of the Using the tube for the administration of food and medications, it must be taken into account that the medications must be crushed and diluted in a way that does not promote obstruction of the tube.Medications with enteric protection or slow release should not be macerated or administered through the tube because their bioavailability changes.It should also be taken into account whether the industrialized diet being used is compatible with the medication since incompatibility can lead to the formation of precipitates.It is recommended to wash the tube before and after each medication and before restarting the diet.(5,6,9)
Through the analysis of the notes made by doctors and nursing professionals in the clinical history, possible signs of complications were identified.The signs indicative of complications were categorized according to the information described in the literature, (,3-,5,6,9,10) which are presented in table 5.


In Table 6 we present the results of the data collected in the medical records analyzed and referring to the sample studied.


The most frequently observed signs were diarrhea (22.2%), vomiting (16.6% of cases), removal of the tube by the patient (13.8%), discharge of the probe (12.9%) and obstruction of the probe (11.1%).
According to the nursing notes, in the face of signs of complications, nursing interventions were carried out that They are seen in table 7.


In the previous table we can see that the nursing interventions carried out against complications are those recommended in the literature.(,3-,5,6,9,10)
Despite carrying out appropriate interventions against complications, the nursing team did not record whether or not they verified the position of the tube (by auscultation, aspiration of gastric contents or pH test) before the administration of the diets, only the tube insertion procedure was recorded.Problems related to the ability to absorb food (diarrhea, dehydration, malnutrition, salmonellosis, short bowel syndrome, diverticular disease of the colon) were responsible for 18.8% of the registered indications.
The signs The most frequent complications recorded in the medical records that indicated complications were gastrointestinal complications, followed by mechanical complications.The nursing interventions that were performed the most were patient hygiene and bed arrangement, decrease in the rate of diet infusion, administration of prescribed medication, and installation of another catheter.Recording of tube position prior to diet administration was not identified in the nursing notes, which could prevent serious pulmonary complications.
To advance nursing practice in this new millennium, it needs to have a strong scientific basis.The practice of administering medications through the nasogastric tube should be based on scientific studies and experiences of specialists for both the prevention and treatment of complications.
Bibliographic References
1.Ahmed A, et al.Esophageal perforation: a complication of nasogastric tube placement.Am J Emerg Med 1998;16(1):64-66.
2. Carrilo E, et al.Intrapleural placement of a nasogastric tube.Can J Anaesth 1998;45 (3):284-285.
3. Waitzberg DL Enteral and parenteral nutrition in clinical practice.Atheneu 1995;206- 213.
4. Eisenberg PG.Pulmonary complications from enteral nutrition.Crit Care Nurs Clin North Am 1991;3:641-649.
5. Kohn CL, Keithley JK.Enteral Nutrition.Potential Complications and Patient Monitoring.Nurs Clin North Am 1989;24(2): 339-353.
6. Thomson HG.“Granny’s Knot” as a complication of nasogastric tube feeding.Ear Nose Throat J. 1989;68(8):639.
7. Kolbitsch C. Pneumothorax following nasogastric feeding tube insertion in a tracheotomized patient after bilateral lung transplantation.Intensive Care Med. 1997;23(4):440-442.
8. Metheny N. Testing feeding tube placement auscultation vs.pH method.Am J Nurs 1998;98(5):37-42.
9. Guenter P, Jones S, Ericson M. Enteral nutrition therapy.Nursing clinics of North America 1997;32 (4):651-668.
10. Lord LM.Enteral access devices.Nursing clinics of North America, 1997;32 (4): 85-704.
11. Murphy JL.Tube feeding problems and solutions.Adv Clin Care 1990;58(2):7-11.
.


Leave a Comment